Dutch doctors worry palliative sedation becomes the norm at the end of life

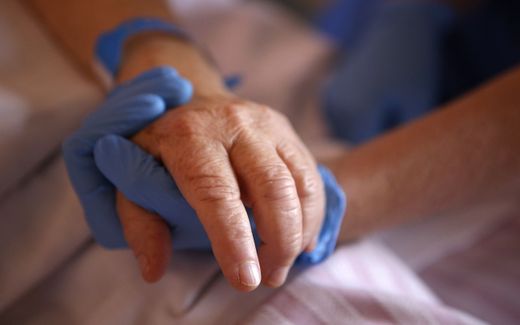
Patient in a hospice unit. Photo AFP, Sergei Supinsky
Western Europe
More and more people pass away while sleeping deeply. Dutch doctors worry that palliative sedation will become a new norm in end-of-life care.
"It seems that dying in your sleep becomes the new normal", hospice medic Maarten Scholten wrote last year in the magazine Medisch Contact (Medical Contact). He argued that Dutch doctors too often choose palliative sedation.
Scholten, who now lives in the United Kingdom, points out to the Reformatorisch Dagblad that palliative sedation is unnecessary in many cases. Whereas in the Netherlands, the practice is part of his standard toolkit, the English medical world only uses sleeping drugs to decrease symptoms. "Only in rare exceptions, we use means like Midazolam to bring people to a continual sleep. That is rarely necessary when you have good palliative care."
He explains the advanced development in England by the fact that the country had started developing its palliative care well before states like the Netherlands did so. "In the Netherlands, we have been busy developing the euthanasia practice first. The attention for palliative care came later." This knowledge gap can, for example, be seen in the fact that there is a specialisation for palliative care during medical studies.
Holistic care
Scholten likes such developments. "I have always supported holistic care, keeping an eye on someone in his whole humanity. In a hospice, you have the time for that. I can sit next to a patient and listen not only to his physical complaints but also to his fears, concerns, wishes and questions about the meaning of life. We can play into this as a team of specialised doctors, nurses and paramedics. Therefore, most people die a natural death here."
In contrast, the physician notices an increase in palliative sedation in the Netherlands. "We don't know whether this is because of an increase in untreatable symptoms or the wish to keep control over the dying process", he says to the Reformatorisch Dagblad. In any case, he is not happy with it. "My main argument against this practice is my view on life. We have been medicalising a lot, from getting children to death, even though all these events belong to the circle of life. And for most people, life ends like a candle, without severe suffering."
Unnecessary palliative sedation does not do justice to essential aspects of the dying process, Scholten says. "Sitting next to the bed, holding the hand of the dying person and exchanging a meaningful smile, these things are all important for processing the loss."
Guidelines
Even though Scholten's article in Medisch Contact led to many hostile reactions, some medical specialists also appreciate his contribution. Family doctor Bertus van Dijk, who also specialised in palliative care in England, is not unhappy with the current guidelines for palliative care in the Netherlands. They were revised last year.
However, one of his concerns is that it includes "intermitting sedation." He argues that offering someone an effective sleeping pill is not sedation. "We should reserve the term sedation for bringing people into a deep sleep because of refractory symptoms for which there is no cure. In the past, this was all about untreatable pain, nausea or unrest. But nowadays, these symptoms can be treated very well. Instead, mental aspects, such as the lack of meaning in the suffering, are weighed heavier. But a practical objection is that this can lead to weeks of sedation."
It often happens that palliative sedation is requested not because of real suffering but because of feared suffering, Van Dijk says. Sometimes, family members find it hard to sit at a deathbed. "It happens that they want more than the medical experts deem necessary."
Marleen Hout, a specialist in elderly care, notices the same thing. "I hear from several family doctors that patients and family members find it obvious that the option of sedation exists. They say: But can't you just be brought to sleep? Then it is hard for a doctor to say that there is no reason for that yet. Sometimes, they adhere to the pressure and administer palliative sedation." The specialist elderly care argues that the goal of sedation should always be easing symptoms, not a deep sleep for the patient.

Rational use
At the same time, Hout finds it too easy to call palliative sedation a form of euthanasia. Instead, she sees it as sedation for false reasons. "The problem is that we cannot handle the death of our loved ones as a society anymore."
Although happy palliative sedation exists, she pleads for careful and rational use. "Too often, people suggest that there are only two ways of humane dying: euthanasia or deep sedation. Those are two extremes. The large majority of people die a natural death without severe suffering."
Pressure
Hout seldom has to apply palliative sedation in the hospice where she works. She notices this is more often the case when people die at home. "It would be good to research where this difference comes from", she says to the Reformatorisch Dagblad. "Is that because of the pressure family doctors experience? Or maybe because of lack of information on the side of family members and the patient?"
The specialist elderly care pleads for a broader approach in palliative care. Symptoms can have many causes, and a family doctor is not specialised in all medical fields, she says. Therefore, she thinks it would be better for them to consult other experts when palliative sedation seems to be a real option.
In addition, the presence of family members and friends can make a real difference, Hout points out. "Many fears and unrest in the last phase of life result from insecurity and loneliness. The feeling of security may be an important reason why we seldom have to sedate in our hospice."
Related Articles