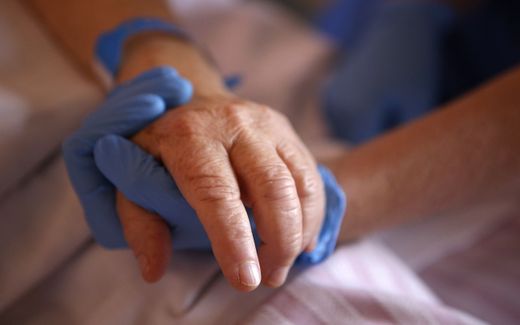
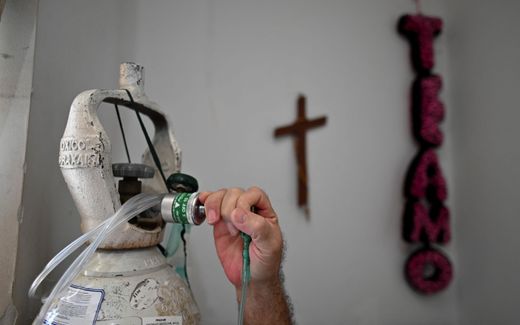Proximity eases suffering at deathbed
16-03-2023
Central Europe
Jonathan Steinert, PRO
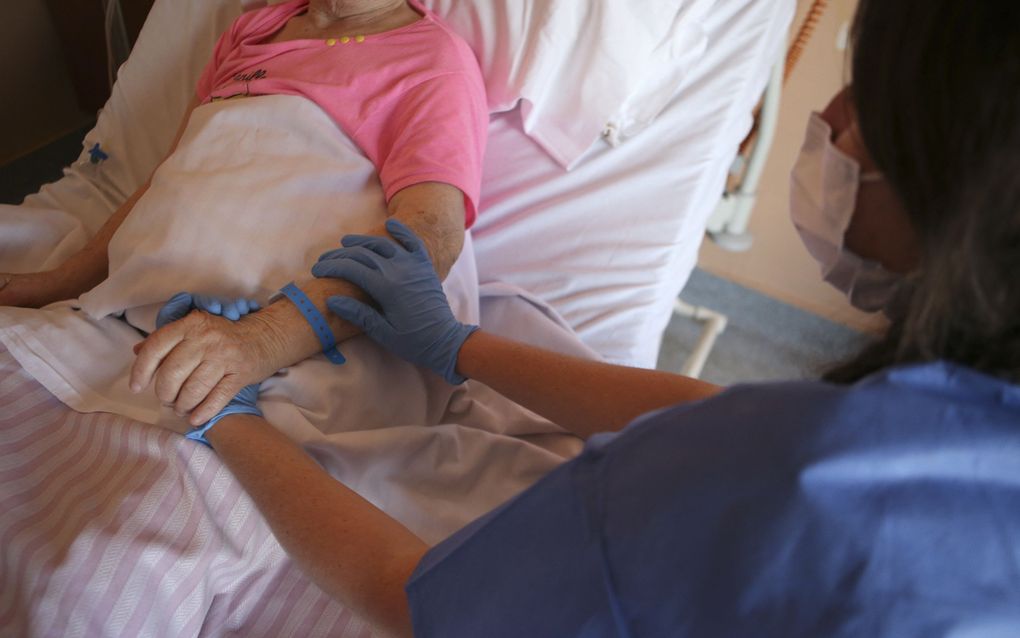
A nurse holds the hand of a patient in the palliative care unit. Photo AFP, Pascal Pochard-Casabianca
Central Europe
Seriously ill people are afraid of suffering. Some, therefore, want to end their lives prematurely. But the suffering can be alleviated. That is what palliative doctors and nurses specialise in. Often there are other needs behind the wish to die.
"I would be happy the end came quickly now," the woman says. She is sitting on her bed in the hospice. From the outside, you can't tell that she is terminally ill. But inside, a tumour keeps growing. By now, she can no longer see well in one eye; the tumour is pressing on the optic nerve. It is cool in the room, which is good for her. She often has the feeling that she is not getting enough air. A device pumps oxygen through a transparent rubber tube into her nose.
Nicolai Deresz squats opposite her, the laptop on his knees. The palliative care specialist asks how she is, what she needs, and how he can help. At the same time, he types on the laptop which medicines need to be ordered. He also documents the visit. Deresz is on the way with his colleague Kerstin Bopp from the Frankfurt palliative team. They had already cared for the woman when she was still living at home.
For the palliative team to be able to help a patient, it needs a prescription from the family doctor. Only then does the health insurance pay for the care. The palliative team sees itself as a cooperation partner of the family doctor, nursing staff, therapists and relatives. It ensures that patients with an incurable, life-limiting illness are well cared for on the last stretch of their lives.

"We enable dying," says Deresz. By this, he means that palliative care does not preserve the patient's life as long as possible medically at any cost. Instead of being in a hospital, people should be allowed to leave life with dignity in their familiar surroundings and as comfortably as possible. It is not about healing but about the relief of suffering.
The doctors and nursing staff of the outpatient palliative care team are available around the clock and visit their patients at least once a week. In doing so, they take measures to make suffering more bearable - for example, by providing medication against pain, shortness of breath, nausea, restlessness, and anxiety. Or they call in someone for care, help in the household, special therapies or people who come to visit.
"30 per cent of our work is medical treatment, 70 per cent is talking," Deresz says. "The presence of people, conversations and physical closeness reduce suffering," explains his colleague Bopp, a nurse with additional training in palliative care.
She repeatedly observes how strained relationships make the end of life more difficult for patients. "The need for conversation is great. We are all in need of healing," she says. Loneliness, in her eyes, is a symptom of an individualistic society that puts the self first. As a result, the sense of caring for others is lost.
Anxiety
A cancer patient whom Bopp and Deresz visit suffers from depression and anxiety disorders. His family cannot find the words to talk to him about his impending death and the life he has led so far. The man's facial bones protrude from under his yellowish skin. When Deresz talks to him, he has to lean close to understand him. The patient mumbles that a conversation with a chaplain would undoubtedly help him.
The palliative team in Frankfurt also includes a staff member who takes care of spiritual care for the patients. This is not paid for by health insurance; the position is financed by donations. When Stephanie Link visits patients and talks to them, it is often about unprocessed feelings of guilt, questions of meaning, about biography. Link wants to guide people to their sources of strength: What has helped them in life before, and what have they achieved?
For some, the question of God also comes into play. Link tells about a 56-year-old woman, mother of two, diagnosed with a brain tumour. She had grown up Roman Catholic but later broke with it. Through her illness, she was able to connect to her childhood experiences and rediscover faith as a source of strength. She built up an intimate relationship with Jesus and finally died, knowing she was not alone.
"We have a deep longing within us to belong and to be held," says Link. A need that a secularised society can hardly satisfy without reference to spirituality. When people say they want to die, Link often sees it primarily as a cry for help – because they are suffering from pain or have the feeling of being abandoned by God and people. "That is immense suffering," she says. That is why this social and spiritual aspect is an important pillar of palliative care.
Ritual
Every morning, the palliative care team members discuss how the patients are doing, how the treatment needs to be adapted, what needs to be organised, and who needs to be informed. The team can look after up to sixty patients in total. On this Monday morning, forty are on the list for the meeting; seven patients have died over the weekend.
Even though the staff deal with the dying daily, the news of death does not easily pass them by. Therefore, every Wednesday, there is a joint ritual in which the palliative team remembers the deceased. Those who wish to do so can share their views and experiences with the former patient. There is also a monthly supervision session.
Bopp remembers the case of a young woman in her early 20s, intelligent, good-looking, sympathetic, and surrounded by her family. "There was so much love around there," says Bopp, fighting back the tears. Bopp and her colleague had admitted her to the palliative care programme; her condition seemed stable. But on their way back to the car, they received an emergency call that the young woman was suddenly getting worse. She died a few hours later.
However, the palliative team can also discharge some patients from their care. They call this "stabilisation". The medication and care are then so well adjusted that the patient is coping or recovering.
A home visit leads Bopp and Deresz to a 97-year-old lady. She was admitted to palliative care a few days ago. A dozen different medicines are piled up on the table. The senior lady sits on the sofa wrapped in a blanket, an empty wine glass beside her. "What is your favourite wine?" Deresz asks her. "Crémant," she answers. She is often tired and often cold, she complains. The doctor explains that this is also due to old age.
During the conversation, it becomes clear that the lady is increasingly unable to take all the medication at the right time and to manage her household. Deresz and Bopp stay with her for almost an hour, call relatives and organise a nursing service. In addition to medical support, the aim is to build up a network for the lady in which she is well cared for. A nursing home is not an option for her. "We want to make you as comfortable as possible," Deresz emphasises.
Lethal injection
It has also happened that patients have asked him to give them "the lethal injection", he says. Then he must first explain to them that this is not the goal of palliative care.
He tells about a patient with a tumour. Her sons planned to travel with her to Switzerland to have her life taken there by a so-called assisted suicide association. Deresz made it clear: "My job is to make suffering bearable. Give me some time to do that." In retrospect, the son admitted that it would have been a mistake to end his life prematurely.

As a Christian, he cannot help anyone to die prematurely for conscientious reasons, says Deresz. But he also thinks, independently of this, that society should not go down this path. For he notes: the wish to die is often an expression of unbearable suffering. "If it can be made more bearable, the direction often changes," he says. Often, physical suffering is also connected to entirely different unmet needs. The art is to recognise these.
This article was translated by CNE.news and published by PRO on March 13, 2023

Related Articles