Working in a hospital during Covid: at the limit of our abilities
11-03-2023
Christian Life
Anna Lutz, PRO
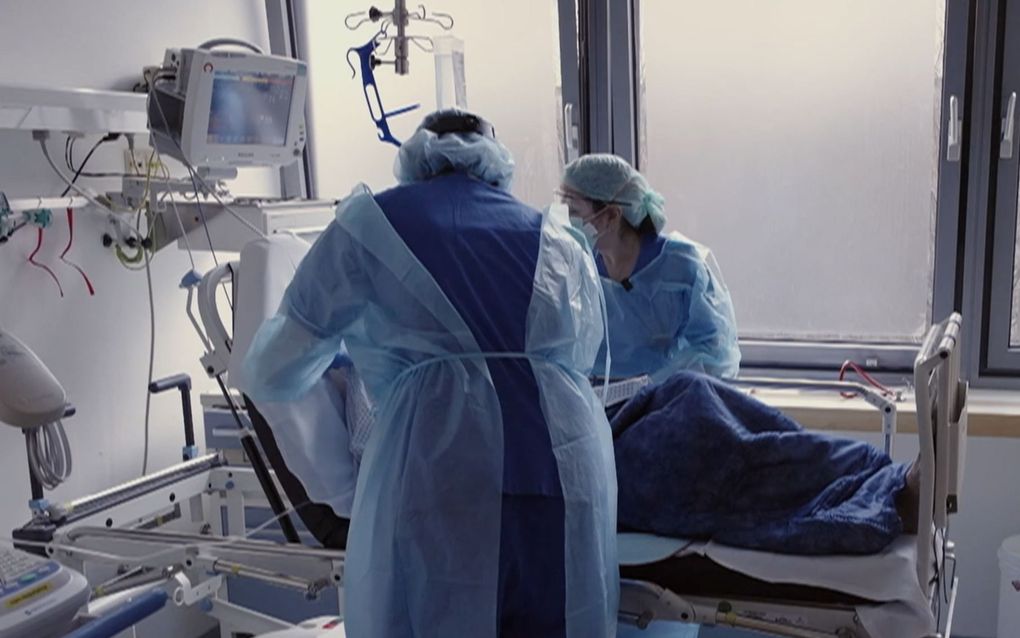
Screenshot showing nurses taking care of a Covid patient in the Charité hospital in Berlin. The image is taken from the documentary "Charité Intensiv". Photo Ardmediathek, rbb
Christian Life
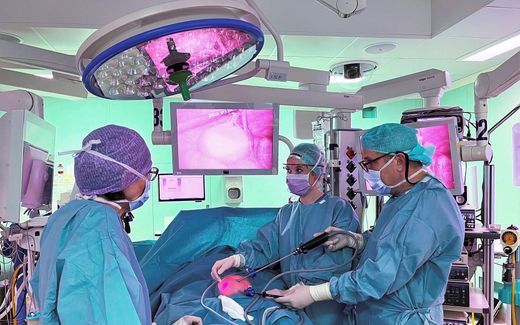
As a senior physician in the intensive care unit of Berlin's Charité hospital, Daniel Zickler has personally experienced every Covid wave. A conversation about faith in times of crisis, hope in the face of death, and love for one's neighbour.
PRO: Documentary maker Carl Gierstorfer accompanied you and your colleagues through the second wave of the pandemic in the winter of 2020. In the documentary ("Charité Intensiv"), it says: "The patients here are dying like flies." Had you ever experienced anything like that as an intensive care physician before?
Daniel Zickler: "Corona was a completely new disease in the first and second wave. The immune system had no protective mechanism whatsoever. The patients got thromboses, haemorrhages, and multiple organ failures. And we had hardly anything to treat it despite ventilation, dialysis and heart-lung machines. Many, many of our patients died.
We, as doctors, constantly had the feeling: We work and work, but somewhere in the body, there is always a new construction site. We had never seen such a heterogeneous clinical picture. We had the impression that the undertakers were constantly in our ward picking up the deceased. We usually only see them every few days.

It also clearly showed us the limits of our abilities: Especially in the case of patients without pre-existing conditions; we had never known them to die before. That was incredibly depressing. On the other hand, we knew: We do what we can and give our best.
Gierstorfer writes in the epilogue to your book "Kampf um jeden Atemzug" (Fighting for Every Breath) about the time he spent filming in the intensive care unit: "It took me weeks to recover from the three months there. Yet I wasn't even remotely exposed to the stresses and strains of the intensive care doctors." What was particularly difficult for you?
"The continuous workload. We intensive care doctors are used to working a lot and even to people dying. But usually, we have rest periods. We can sleep for twelve hours and then continue the next day. But during the pandemic, we were on duty sometimes until three in the morning and then called back on duty at eight in the morning. And that was for many days at a stretch.
Besides, it was all very emotionally exhausting. Because so many people died, we had to inform many relatives; it was insane pressure. And then we were also in a state of exhaustion. Today I can hardly believe that we got through it."
Have you ever had to decide on the life and death of a patient in a pandemic?
"We doctors always had in the back of our minds that triage could happen, but it never did. In Germany, unlike in many other countries, we could provide absolute maximum care to everyone: We ventilated all patients who needed and wanted it. Everyone got a fair chance; I'm sure of that. And that is a great credit to all the staff in intensive care units and to society as a whole.
But it is also clear: it was close. There couldn't have been many more patients. Then we would have been overwhelmed and would have had to turn people away. We have already paid a high price as it is. Nevertheless, I think we were right to prepare for even worse scenarios. Because there were worse scenarios in other countries and we didn't know what was coming in Germany.
At the same time, the child and youth psychiatries were suddenly full - presumably also because of the burdens of contact restrictions and other Covid measures. Was it worth it?
"We will think for a long time about which measures were correct and which were not. We already suspect, for example, that the daycare centre closures may have been a mistake. But how could we have known all this at the beginning of the pandemic?
In Germany, 160,000 people died of Corona. This number would have been significantly higher if we had not taken any measures. The pandemic had many negative effects on society. However, it has not been proven that all mental problems were solely due to lockdown measures. Many people became seriously ill from the virus, which may also have contributed to it. But of course, there were measures that, in retrospect, did not make sense."
Which ones?
"We now know that the risk of infection outside is quite low. There, the need for contact restrictions was actually low. For me, closing off playgrounds is one of the measures that did not make sense."
You write in your book that you believe in God. Have you ever asked yourself why He allowed this suffering?
"I have never asked myself why God allowed this to happen. From my point of view, that is the wrong question. There are things in this world that are not just. But being a believer helps in every profession, especially in mine. I know that I am fallible, even if I do my best. And I can trust that God will stand by me."
There was massive resistance to the corona policy and measures against the virus during the pandemic. Christian groups were also involved. What would you like to say to them?
"I would say: 160,000 people have died, and many have become very seriously ill. I think masks have protected us, and you are on the wrong path."
Have you met such Christians in your environment?
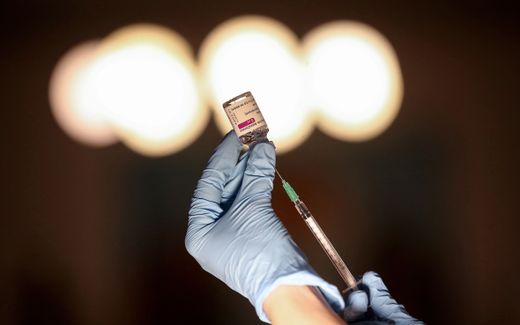
"No. Our congregation closed very quickly in the first wave and switched to online services. When we started meeting again, it was clear: wearing masks and keeping our distance and later vaccination; all these are acts of charity, and we stuck to them. That is also my personal opinion.
Of course, I have met someone here and there who said: I have faith in God; I don't need a vaccination. I can't understand that. No one sits in a car without brakes because of their trust in God."
In the first wave of Covid, the churches were closed, and, as the pandemic progressed, many services were cancelled, and singing was forbidden. Was that justified?
"Churches have an essential function, especially for lonely people. It was right to reopen them early, but that doesn't change the fact that there was a risk of infection to which the visitors were exposed. It was good that we were careful and wore masks. Was every single measure right? I don't know. But that discussion is also idle."
People died alone in old people's homes and hospitals because they were not even allowed to receive companions for the dying. Relatives were not allowed to see their terminally ill spouses.
"In the Virchow Hospital of Charité, where I work, relatives were always allowed to say goodbye; you can see that in the documentation. I know that there were very strict conditions in many hospitals. We were careful, but one person was always allowed to come for one hour a day for seriously ill patients. With protective equipment, that was also doable.
The only exceptions were when relatives were in quarantine. Otherwise, every patient could have a visitor. In retrospect, I would say that they could have been more liberal elsewhere. On the other hand, in nursing homes, such measures also prevented the grandson from infecting the grandmother and causing her to die."
Two scenes from the documentary "Charité intensiv" have particularly stayed on my mind. There is Marco, who struggles back to life after being ventilated and whom you were able to discharge. And a man whose wife sings praise songs and prays at his bedside. And yet he dies. What did these two stories do to you?
"These two stories have shown that it can go one way and the other. Both patients were affected similarly. Both received the same therapy. Both had similar conditions. But only one made it.
A sense of achievement like Marco Wegner's was crucial for us as doctors. It showed us that not everything is in vain. The other example was particularly moving. The whole family was at the man's bedside. His wife had enormous faith in God; she believed until the end that her husband would make it.
That's why it was also very difficult for me to assess the situation realistically for her. I had to tell her: He probably won't make it. And that without taking away her trust in God. That was very difficult. But it was also quickly noticed that she could process everything very well. She still said thank you at the deathbed of her husband, to us doctors, but also to God for her husband's life."
In December 2021, you appeared on the TV programme "Joko und Klaas" together with Chancellor Olaf Scholz in front of millions to promote vaccination. How did you experience that?
"It was on my day off. The press officer of the Charité called me and said: I have something for you. Of course, I was excited. There was no script and no teleprompter. But the team was super nice, and so it went well. The reactions were mostly positive. My son came home from school a short time later and excitedly told us we were number 1 in the YouTube trends."
In your book "Kampf um jeden Atemzug" (Fight for Every Breath), you lament the exodus of numerous nurses and doctors because of poor working conditions in hospitals. After almost three years of the pandemic: Would you take up your profession again in the current situation if you had the choice?
Absolutely. For me, it is a calling. I can help people in difficult situations and work in a team, and there is a bit of action as well. Even during the pandemic, I realised how I could use what I learned to save people. That's great, despite all the difficulties and stress."
What drives you?
"I have the opportunity to practise charity. My family helps me. And my faith."
Every day at work, you stand on the threshold between life and death for your patients. Have you ever experienced a miracle?
"In the documentary, there is a moment when a patient suffers a cardiovascular arrest during the emergency placement of the heart-lung machine. I thought a lot about that afterwards. The fact that we managed this emergency so well is a miracle for which I am incredibly grateful.
In my 15 years in the intensive care unit, I have repeatedly encountered patients of whom I thought: They don't stand a chance. And then, they left the ICU on two legs. I would call that a miracle, and it moves me every time.
I also never thought that we, as doctors, could go through the stresses of the pandemic without breaking down. The fact that we managed to do that and that many of us are still going on now is really remarkable. However, I also know colleagues who have said: We can't continue any longer."
This article was translated by CNE.news and published by PRO on February 26, 2023
Related Articles