How do Christian hospices deal with a death wish of their patients?
06-11-2023
Christian Life
Maarten Costerus, RD

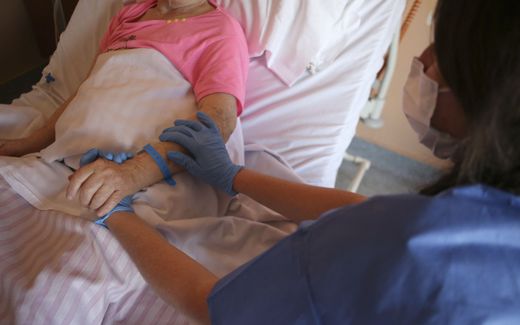
An elderly hospice patient in a wheelchair. Dutch hospices do not often get a request for active euthanasia, but sometimes they are asked about the possibility of passive euthanasia. People want to hasten their death by stopping their food and drink intake. Photo EPA, Peter Komka
Christian Life
Now and then, Christian hospices are confronted with an elderly person's wish to die by stopping their intake of food and drinks. They deal with this differently.
Most hospices offer counselling to people who consider their lives complete and want to die by stopping eating and drinking, research by the Dutch broadcaster Nieuwsuur among some 40 hospices revealed at the end of September. According to the current affairs programme, there is increasing interest in this way of dying.
However, the increase is not supported by figures from the Dutch statistics agency CBS. In the most recent CBS survey from 2021, the numbers were too low to make an estimate. In 2015, it was 0.5 per cent of the total number of deaths in the Netherlands, equivalent to over 700 people. By comparison, 4.5 per cent of deaths in that year involved euthanasia. And 0.2 per cent ended their lives by taking lethal drugs.
Christian institutions are occasionally confronted with people's wishes to die by no longer eating and drinking. "We get such a request several times a year," says Jacomijn Wittenberg, nurse and manager of the Christian hospice De Wingerd, part of healthcare organisation Charim, in the Dutch town of Amerongen. "That is slightly more often than before."
Emotions
People who are terminally ill and indicate they want to stop eating and drinking can come to De Wingerd says the manager. "We feel it is our duty and calling to care for dying people, whatever the reason for their approaching end of life. However, it can be intense when we have to accompany someone who is hastening their death themselves. We try to put those emotions aside. This person has made that choice, and we respect that. In the team, we pay attention to colleagues with conscientious objections. We have a conversation about that together."
The desire to die often comes from a lack of meaning, Wittenberg believes. "These people ask themselves: what am I still living for? Every day feels the same; every day, they are in pain. Moreover, they are often dependent on others, such as family and caregivers. There are also those who say: my life has been complete; why should I live any longer?"
Attention
The nurse believes that many wishes to end life shift to the background when people feel safe, loved and given due attention. "I believe in the power of a circle of people, from the family or church, around an elderly person. But even then, someone can see their life as completed. I have seen situations where people had decided to stop eating and drinking and where the family lovingly supported them in this process."
Why don't these people choose euthanasia, the active termination of life? "Not everyone wants to go through such a process and burden others," explains Wittenberg.
Injection
The nurse sees a fundamental difference between euthanasia and stopping eating and drinking. "It makes a big difference whether the professional actively ends someone's life or the patient himself shortens his life span by not taking any more food," she says. Charim does not cooperate with euthanasia or assisted suicide. “We always want to care for the patient but will never give him a lethal injection."
Wittenberg and her colleagues adhere to national guidelines which, among other things, prescribe how much water a patient can be given in case of dry mouth without disrupting the dying process.
Isn't it tempting to give someone more water to keep them alive longer? "If someone does not want to, it is wrong to do it anyway," Wittenberg says. "I myself wonder in such a situation what Jesus would have done."
Alert
Sometimes, it happens that people become confused due to lack of fluids and still want to drink something. How do nurses at De Wingerd deal with this? Wittenberg: "If someone specifies in advance that they do not want water when they are confused, we respect that and stick to those agreements. That is not always easy. For that matter, someone can always withdraw his decision. If he says in full consciousness that he can no longer bear the conditions –which sometimes happens– we certainly don't hold that against him."
When a person stops eating and drinking, he gets weaker and weaker and becomes dehydrated, the nurse explains. "At some point, due to fluid deprivation, he becomes less and less alert and slumps. Eventually, the organs stop functioning, and the person dies."
Valuable
Christian hospice De Regenboog in the Dutch town of Nunspeet has a different policy: it does not take in people who want to die by stopping eating and drinking. "If we get a registration from someone with that wish, we first enter into the conversation," says director Gerrinda van der Veen. "We then ask how someone came to that choice. At the same time, we indicate that we see life as valuable from beginning to end and cannot support a self-chosen end."
Hospice Ede De Olijftak also does not cooperate with requests from people who want to end their lives due to dehydration and starvation. "We do not consider that an indication for hospice care," explains team leader Lia van Laar.
It sometimes happens that people indicate during their stay in a hospice that they no longer want to eat or drink. "With us so far, these are almost only people who are in very bad shape and say: I can't take any more," Van Laar says.
Gasp
It is increasingly common for elderly people to consider their lives complete and want to die by euthanasia or by refraining from eating and drinking. "This is part of a trend where people want to take their dying into their own hands," says Diederik van Dijk. He is the president of NPV Care for Life, a pro-life organisation in the Netherlands. "This is self-determination to the last gasp and is not unrelated to secularisation. People do not want to wait for the last breath determined by the Higher Power."
Worryingly, Van Dijk finds that GPs are increasingly actively suggesting the option to stop eating and drinking to people who are tired of life these days. According to him, this is the latest trend.
Conversations
This option, which also involves hospices, he says, has a threshold-reducing effect. "Suppose someone with psychological needs does not get through a euthanasia process and then reports to a hospice with a request to die there by stopping eating and drinking. What review then takes place? Or does it stop at one or two conversations?"
The NPV director, therefore, has a "full understanding" of hospices that do not want to cooperate with a patient's request to die by not taking any more food and drink. "Hospices that do so are facilitating someone's death wish. That is not what they are meant for, and this damages the sense of security people want to experience in a hospice."
Van Dijk has fundamental objections to ending life by refusing food and drink. According to him, this choice is not compatible with the sixth commandment, "Thou shalt not kill".
Refuse
"Self-elected mortification we reject unreservedly," says Rev G.F. Willemsen, spiritual counsellor and chairman of an ethics committee of the organisation hospice De Wingerd is also part of. "Life comes from God, and in our view, it is not up to a person to take the initiative for the end of life."
"Yet we don't readily refuse care when a terminal patient calls on us," the pastoral worker continues. "Not even if the dying process is caused by the patient himself. Mercy wins over judgment, then." Employees who do experience ethical problems can be replaced by a colleague, according to the pastor. "We guard the freedom of conscience of our staff," he said.
Rev Willemsen emphasises that hospice De Wingerd takes in only terminal patients. "There is no possibility with us to be admitted as a non-terminal patient with the aim of initiating the dying process within our hospice."
This article was translated by CNE.news and published by the Dutch daily Reformatorisch Dagblad on November 4, 2023
Related Articles